Serving Michigan's rural communities
Clinical placements, traineeships address critical shortage of health care providers
by Michele Coffill
photos by Amanda Pitts, unless indicated
video by Tony Packer
Ali Saheb grew up in Grand Marais, a small village on the shore of Lake Superior in the Upper Peninsula. He graduated from high school with six other people.
Saheb earned a bachelor's degree in nursing in 2011 while living in the U.P., then accepted a job in the neurovascular unit at Bronson Methodist Hospital in Kalamazoo. He enrolled in the Kirkhof College of Nursing to begin the doctor of nursing practice (DNP) program; in September Saheb started working at another hospital with a population that resembles his hometown. Saheb said reclaiming a sense of community in his life played a role in the decision to switch gears.

Ali Saheb
He is one of 14 DNP students who each received a $22,000 traineeship grant to work in a rural setting for a year. "I understood what it meant to be in a rural community, and helping people who really need it was something my family had instilled in me," Saheb said.
KCON earned a one-year, $332,640 Health Resources and Services grant, from the U.S. Department of Health and Human Services, to train and prepare nurse practitioners to work in Michigan's rural communities.
Karen Burritt, associate dean for graduate programs, said the grant enables KCON to address the critical shortage of qualified health care providers in rural areas. Burritt and Sandra Spoelstra, associate dean for research and scholarship, wrote the grant, and the fact that they are both originally from the U.P. is not a coincidence.
"My family still lives in the U.P. and I know the difficulties of coordinating care and having access to specialists," Burritt said. "I knew our DNP students could make a positive impact."
Lakeland Hospital, Niles
Not all traineeships involve direct patient care. Saheb, a fourth-year DNP student, is working on an administrative project that could bring systematic changes to Lakeland Hospital and Lakeland Health, the parent organization that serves Berrien County and southwestern Michigan.
He is working with nurse practitioner Sonya Christensen to create a sustainable model for transitions of care management, a health care term that refers to moving a patient from one setting to another — from a hospital to a rehabilitation facility, for example. Their project focuses on chronically ill patients who have recurring hospital visits.
Christensen, who earned a DNP from Grand Valley in August, said hospital administrators across the country are watching an ever-changing bottom line because of how Medicare reimbursements work. "Reimbursements of certain diagnoses are not made to hospitals by Medicare if the same patient is readmitted with the same diagnosis within 30 days," she said, adding that bundled payments under the Affordable Care Act may change the time period to 90 days.
She started working on a transitions of care model before Saheb joined her by creating a database of Lakeland's chronically ill patients — people with congestive heart failure, acute cardiac problems — and their re-admittance rates. Once the analysis is complete, Christensen said it will support a proposal to hire additional staff to make home visits to patients for 30 days after their discharge date to ensure medications are being taken and they are following their health plans.
"I began to see this problem daily. I was getting these patients who were frequently admitted," Christensen said. "As a nurse practitioner, it was clear to me what the issues were, including that there wasn't follow-up care."
"This is the essence of being a DNP. It's going through processes and assessing an organization by looking at its strengths and weaknesses." Ali Saheb
Saheb called studying organizational and systems-level changes "the essence" of being a nurse practitioner or, in his case, a student studying advanced practice nursing.
"This is the essence of being a DNP. It's going through processes and assessing an organization by looking at its strengths and weaknesses," he said.
Saheb was caring for stroke patients at Bronson Hospital before earning the traineeship grant and traveling one hour several times a week to work with Christensen in Niles. For his doctoral dissertation, he had planned a project in Bronson's neurovascular unit. Then he got word of the rural health care grant.
"Staying at Bronson would have been very comfortable for me. This move helps me grow, and Sonya has been pivotal during these first few months. It's absolutely an ideal situation, she's an expert in the field," he said.
Beaver Island and Peshawbestown
KCON faculty members emphasized training and educating students to practice in rural settings long before they received the federal grant in September, and Megan Madole was among the students who benefited from that early work.
Madole spent the summer of 2016 learning and practicing in two northern Michigan clinics. She was the first Grand Valley DNP student to work at the Peshawbestown health clinic, which serves the Grand Traverse Band of Ottawa and Chippewa Indians; and then worked at the health center on Beaver Island.
Tribal clinic administrator Ruth Bussey said collaborating with KCON to create a clinical placement for a DNP student benefits the community. "It's one more way we can provide our patients with the health care and resources they deserve,” she said.
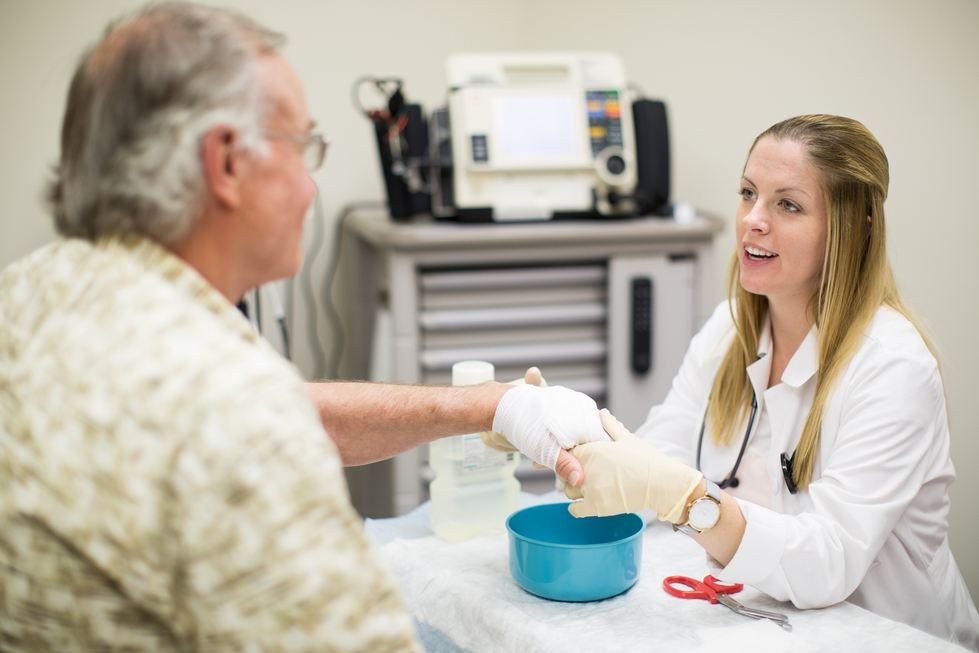
Megan Madole works with a patient at the Beaver Island Rural Health Center.
Madole, who lives in Traverse City, said working at the clinic fully leveraged her DNP training, as nurse practitioners care for the whole patient and consider how factors like race, education and income impact the health of a patient. Madole worked closely with KCON faculty members and Bussey on cultural orientation prior to starting her work at the clinic.
"Working at the tribal clinic was an invaluable opportunity to better understand rural health, the unique challenges rural communities face, and the importance of culture," she said.
Madole's placement on Beaver Island was the start of a partnership between KCON and the health center, and paved the way for other Grand Valley students to follow.
Beaver Island is a popular summer tourist destination in Lake Michigan; most visitors arrive by ferry — a two-hour ride — or airplane from Charlevoix. During the summer, the island's population swells from 600 year-round residents to 5,000.
The health center is operated by nurse practitioners, which Burritt said makes it a perfect clinical partner for Grand Valley. "It's run by nurse practitioners who are eager to help rising nurse practitioners while also learning from them," Burritt said.
Madole stayed on the island in a guest house owned by Don Spencer, a member of the health center's board of directors. He said board members enthusiastically supported the partnership with KCON.

Megan Madole, center, is pictured with KCON staff members and, at right, Donna Kubic and Don Spencer from the Beaver Island Rural Health Center.
"It’s terrific," Spencer said. "The students have experience in outreach, and getting someone to serve on Beaver Island is tough, it's so isolated, and it places a burden on staff and budget. Maybe over time, through one of these students, we will find a new staff person."
Two physicians hold office hours at the health center twice a month and specialists like John Martin, a retired orthopedic surgeon, make weekly visits to see patients. Donna Kubic, managing director, said the staff can see about 20-25 patients daily in the summer and less than five a day during the winter months.
Madole said she enjoyed the mix of tourists who needed acute care for dog bites or bee stings and the year-round residents who needed preventive care.
"It's been very interesting to see how a nurse practitioner has developed such a role in rural health and how health care is delivered," she said. "During an assessment of a patient, we're utilizing their whole history and taking the time to hear their entire story."
Dickinson County Memorial Hospital, Iron Mountain
Jeff Bird earned a DNP in 2014, following a six-year career in the Marines and a job managing a fitness club. "I used to think that nursing was only for women, it was very stereotypical of me," he said.
Bird earned a bachelor's degree in health science and was content managing a fitness club until 2008 when the economy fell and among the first thing people eliminated from their budgets was gym memberships. A friend suggested he might like nursing as a career.
He earned a bachelor's of nursing degree from Grand Valley in 2009, then a former professor suggested Bird continue his education and gave him an application to the DNP program. During that time, Bird was working at Spectrum Health Butterworth Hospital in Grand Rapids, first in cardiovascular care then the emergency department.
To support his doctoral education, Bird earned a different grant that required him to work a number of years in a rural setting after graduating. This led him in August to move his wife and four of his six children from Allendale to Quinnesec, outside of Iron Mountain.

photo by Karen Burritt
Jeff Bird is pictured with Karen Burritt, KCON associate dean for graduate programs.
At Dickinson County Memorial Hospital, Bird splits his time between the emergency department and urgent care clinic. Because of the lack of medical specialists in the region, some residents use the clinic as their primary care provider.
"There are much fewer resources here," Bird said.
Yet like Saheb, Bird is making systems-level changes, on big and small scales. While working for Spectrum Health, Bird was instrumental in developing a policy to identify veterans who were admitted to the hospital.
"My dissertation was on suicide screening at the primary care level for veterans," he said. "Now at Butterworth, there is a system in place to identify veterans and link them, if needed, to community resources."
He is advocating a similar policy be instituted at Dickinson. On a daily, practical level, Bird noticed that the hospital hand sanitizers are placed inside patient rooms. At Spectrum, they were positioned outside of rooms, allowing health care workers to sanitize hands before meeting a patient. Bird said it's a small thing, but he suggested moving the sanitizers outside of patient doors.
"If there's a problem you notice as a nurse practitioner, you have the skills and the tools to bring evidence-based care and make changes," he said.
